Randy Jacobs, M.D. Patient Education
To return to the Patient Education page and read more articles, click here.

Diabetic Skin
The Skin in Diabetes
What
is Diabetes?
Diabetes is an endocrine (hormonal)
disease in which the body loses the ability to maintain normal levels of sugar
in the blood. There are two kinds of diabetes:
1)
Type I, or insulin-dependent diabetes mellitus (IDDM), is characterized by it
beginning in
childhood and requiring insulin shots for treatment.
2)
Type II, or non insulin-dependent diabetes mellitus, is characterized by
running in families,
by occurring more commonly among obese individuals, and by being able to be controlled by medication taken by
mouth.
Since blood glucose is the major nutrient
for many organs, including the brain, it is not surprising that diabetes causes
a variety of manifestations. For example, as a diabetic you have a much higher
probability of developing progressive kidney disease. Atherosclerosis, or
hardening of the arteries, is accelerated in individuals with diabetic. The
nervous system is affected leading to, among other things, decreased sensation.
Even the eyes are affected, making diabetes a leading cause of blindness in
this country. With this background in mind it is not surprising that diabetes
would exhibit manifestations in the skin.
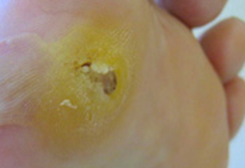
Diabetic
Foot Ulcers
One in five diabetics who are
hospitalized are admitted because of diabetic foot
complications, thus making them a significant problem. Diabetics have poor
circulation due to atherosclerosis of the larger arteries supplying the foot
and leg, which decreases the diameter of these vessels. The smaller blood vessels
are also affected, as diabetes causes them to thicken and eventually occlude.
Superimposed on these factors is the decreased sensitivity of the nerves
supplying the lower extremity. This means that a
diabetic is more likely to injure the foot, even severely, without being at all
aware of it. Diabetics have been known to walk all day long with objects the
size of plastic toy cars in their shoes, only to discover them at the end of
the day. When a diabetic suffers from an injury that breaks the skin, they can
take a very long time in healing, and are predisposed to having severe
infections in their feet because of the poor blood supply and the decreased
resistance to infection associated with the illness. Not uncommonly they
progress to gangrene. Moreover, infections put the diabetes out of control by
often causing tremendous elevations of blood glucose. With this in mind it
becomes clear why prevention is paramount in the care of the diabetic foot.
Footwear must be comfortable, and must be inspected always before use. The feet
must be inspected thoroughly daily to detect any break or injury to the skin.
They should also be kept clean. Smoking must stop, as nicotine reduces blood
flow in the small arteries. Extreme care must be exercised with every minor injury
until it heals. If they don't, or if there is fever, or abnormal elevation of
blood glucose, the physician must be contacted immediately. These same
considerations apply to the skin covering the stump of an amputated extremity.
Treatment involves antibiotics, meticulous wound care, medications to improve
blood flow. Sometimes skin grafting, and the use of
oxygen to speed healing are used.
Skin
Manifestations of Diabetes
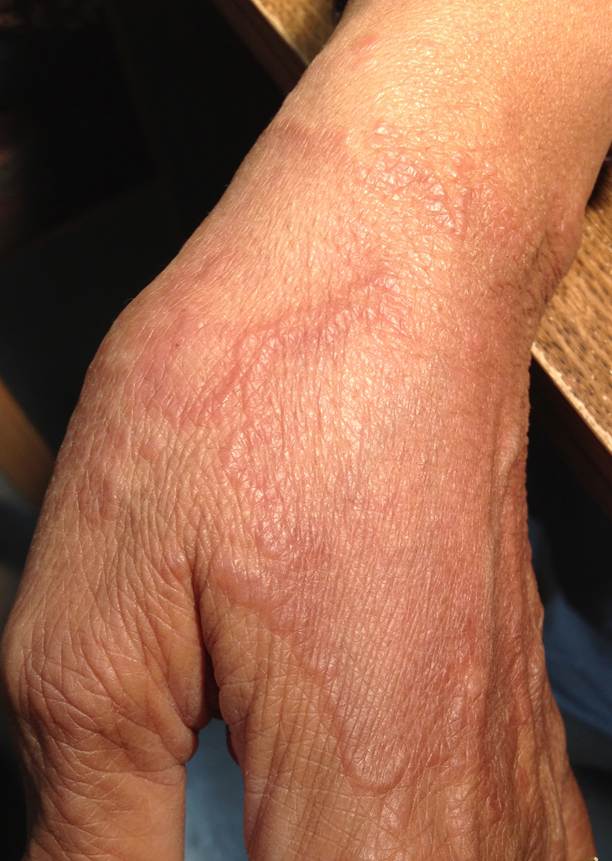
Granuloma
Annulare
This is a benign skin conditions
characterized by raised dome-shaped patches of reddened skin that often assume
an annular shape. It commonly affects the back of the hands and the top of the
feet. It occurs more commonly in women, and in most cases it appears before an
age of 30 years. As it is true of other skin conditions, granuloma annulare is
not caused by diabetes, but it is more frequently found in diabetics. It also
occurs after insect bites, sun exposure, and injury. The lesions resolve within
two years in more than half of all patients (80 %), However,
there is a small subset of patients in which the condition may be chronic.
Treatments to control the condition include steroids, excision, ultraviolet
light, and liquid nitrogen.
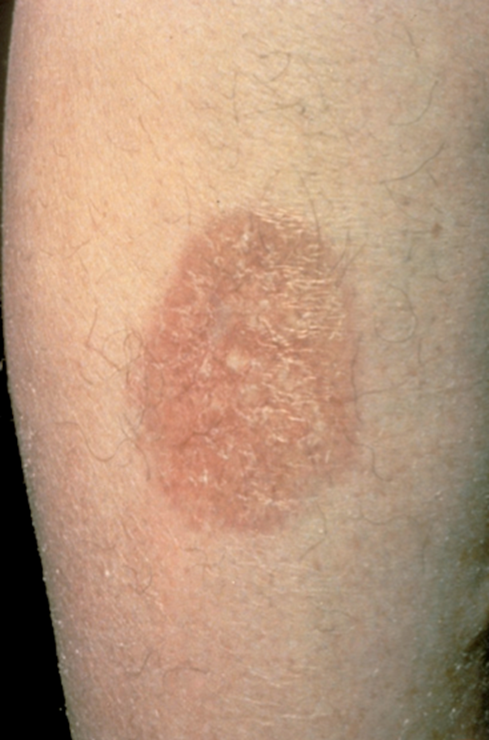
Necrobiosis
Lipoidica Diabeticorum
This lesions occur three
times more commonly in women, and are usually on the anterior and lateral
surfaces of the lower legs. The lesions are small, dusky red, elevated, with a
sharp border. It slowly enlarges, becomes irregular in outline, flattened, and
eventually leaves a thin, shiny skin. The condition is associated with
diabetes. Treatment is very important and consists of steroid creams
injections. Aspirin and medications to improve blood flow are also helpful.
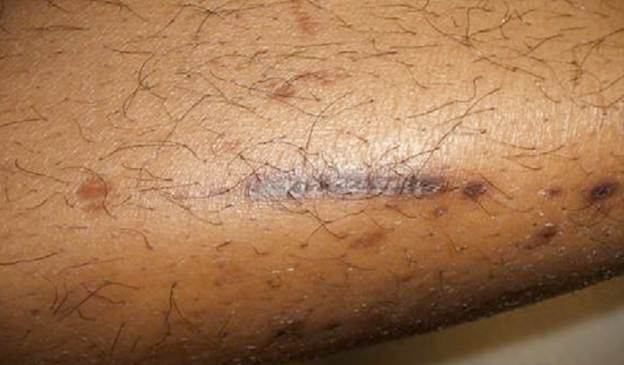
Diabetic
Dermopathy
This condition is defined by multiple
brown shallow scars in the anterior part of both legs. Lesions have sharp
borders to the normal skin. It is the most common skin condition in diabetes,
and most patients who have it are diabetic. It occurs more commonly in adults,
males, and in people with severe or long-standing diabetes. It is not known
what causes diabetic dermopathy, but injury as well as poor
circulation are contributing factors. This c ondition is
harmless and requires no treatment. In people who receive injuries to the
shins, protection is appropriate. In non diabetics, the physician should be
alert for hidden abnormalities of blood glucose control.
Diabetic
Bullae
They are a distinct diabetic skin
condition manifested by large blisters that appear suddenly in legs and arms,
especially the lower leg and forearm. Lesions remain for up to six weeks, dry,
and usually heal without scarring. Both sexes are equally affected, and all
patients are diabetics. Generally no treatment is necessary. Large and tense
lesions can be drained, and managed with topical antibiotics.
Acanthosis
Nigricans
This lesions is
characterized by a darkening and thickening of the skin, which also acquires a
velvety appearance and texture. It is found in the armpit areas, groins, and in
other places where skin is in contact with skin constantly. Control of obesity
may cause regression.
Skin
Infections
Skin infections of many kinds are more
common in diabetics. An in-depth description of each is unnecessary. However,
any infection of the skin that does not heal in reasonable time should be
evaluated
Rubeosis
This is a harmless red coloration of the
face found sometimes on diabetics.
Conditions
Associated with Insulin Injections
The diabetic may
develop allergies to insulin that often become manifested in the skin.
Switching to human insulin may resolve this complication. Also, failing to
alternate the injection sites can lead to both loss of fat, or to an abnormal
growth of fat in the area. Logically, it is best to rotate injection sites for
prevention.
DIABETES: INJECTION SITES FOR INSULIN
- It is important that you be able to give
yourself all your injections, so sites of injection should be selected that you
can reach. Occasionally, if you wish, someone else may inject insulin into your
arms or buttocks.
- The same general area for an injection
should be used no more often than about once a month. Injections into the same
spot will prevent the insulin from being absorbed well, so you will not get
full benefit from the insulin.
NOTE: You may obtain additional information in
greater detail from:
AMERICAN DIABETES ASSOCIATION, INC.
2 PARK AVENUE
NEW YORK, NY 10016
|