Randy Jacobs, M.D. Patient Education
To return to the Patient Education page and read more articles, click here.

Urticaria
HIVES (URTICARIA)
What are the Symptoms?
 Hives are an allergic response of the skin causing crops of raised, red, itching areas, which may come and go. The crops may last for a few minutes or hours, may disappear, and may break out in another location. They have sharp, serpent-like borders surrounded by a red halo in the adjacent skin. The most intense hives have a white or blanched center. Hives range in diameter from several millimeters to over 1 inch. Individual hives last for no more than 8 to 12 hours. However, during the interval of one attack, they characteristically appear and disappear in different places on the skin. Bumps that remain for more than 24 hours in a given spot are not true hives.
Hives are an allergic response of the skin causing crops of raised, red, itching areas, which may come and go. The crops may last for a few minutes or hours, may disappear, and may break out in another location. They have sharp, serpent-like borders surrounded by a red halo in the adjacent skin. The most intense hives have a white or blanched center. Hives range in diameter from several millimeters to over 1 inch. Individual hives last for no more than 8 to 12 hours. However, during the interval of one attack, they characteristically appear and disappear in different places on the skin. Bumps that remain for more than 24 hours in a given spot are not true hives.
Acute and Chronic Urticaria
Hives cause intense itching and stinging. The typical attack of hives lasts no more than several days and often less and is known as acute urticaria. An attack lasting more than 6 weeks is called chronic urticaria. Acute urticaria is usually a type of allergic reaction that occurs, and then resolves within six weeks. More severe symptoms can occur. Hive-like reactions are not always limited to the skin. The same type of inflammation can occur in other parts of the body the windpipe (trachea), voice box (larynx) and air passages (bronchi). When inflammation occurs in these sensitive structures, obstruction to breathing can occur. Some individuals who are allergic to certain foods such as shrimp or lobster can have, in addition to hives, acute difficulty in breathing, which calls for emergency measures similar to those for acute allergic reactions to insect bites.
What Causes Hives?
Please read the following carefully and notify Dr. Jacobs if you suspect anything that could be causing your hives. Think about anything you touch or eat. Ask the receptionist for a copy of the ABC Booklet to learn how you can avoid allergies.
Hives can be a reaction to some environmental factor such as an insect bite, a food (shellfish are a notorious cause), a medication, or as one part of the reaction to many different allergens. Pollens in the air and other air borne chemicals and agents can cause hives.
The factors, which cause hives, may be drugs, foods, injected medications (Aspirin, Motrin, Advil), insect stings, physical factors, such as cold, heat, exertion, and light products of infection, digestive disturbances, and emotional factors. Substances used in cigarettes, cosmetics, hand lotions, contraceptives, toothpaste, gargles, and scalp applications are possible causes of hives.
Part of your treatment is to keep a diary of the foods you eat, the personal items you use, and the medicines you take, the time and occasion when you break out, and the duration of your lesions.
Simple hives are commonly associated with the eating of an unusual food such as a dish of strawberries, or a delicious deviled crab. Hives come almost each time such foods are eaten, particularly if alcoholic beverages are consumed with the meal. Other foods to be suspected include eggs, chocolate, nuts, fresh pork, cheese (except cottage cheese), tomatoes, navy beans, cabbage, onions, mushrooms, grapes, pineapple, fresh berries, fresh fruits, oranges, grapefruit, lemons, ginger, pepper, tea, coffee, mint, spices, menthol. It is obviously impossible to eliminate all such foods under ordinary circumstances. Thus, we make the suggestions with the understanding that if you can associate the eating of any of these foods with the hives, this may be important.
Penicillin, Aspirin, and sedatives are the most common medications, which cause hives. However, most other medications can also cause hives including laxatives, eye drops, vitamins, etc.
Infections such as dental abscesses, tonsillitis, sinusitis, cystitis, cholecystitis, and ringworm, can cause hives. Viral infections are second only to drugs as a cause of hives in children. The infections may be mild or may even be overlooked.
Emotional stress and strain are very frequent causes of hives. In most patients the emotional problems are very well concealed, and it is only with great difficulty that a patient can relate emotional causes to his or her skin problem.
Chronic Urticaria
Patients with a personal or family history of asthma, hay fever or migraine headache seem to be susceptible to stubborn, chronic hives. Once the cause is identified, the best advice is to avoid subsequent exposure to it if possible. Please understand that the cause of chronic urticaria is not identifiable in as many as 70 to 85 percent of cases. Known inciting causes of chronic urticaria include drugs and, less frequently, foods, inhalants, like pollen, and infestation with parasitic worms. Stress and anxiety are often thought to be important factors.
 Another type of hives is cholinergic urticaria, triggered by emotions, heat, exercise, or change in temperature. Cholinergic type is different from the allergic type and is more fleeting in its appearance and disappearance. They are small (1 to 3 millimeters), pinpoint-like, raised wheals, surrounded by a large, intensely red rim. They disappear without treatment in 30 to 60 minutes, but tend to recur in susceptible individuals. Why some people react with hives to stress is not known. Despite the most diligent of efforts, the cause is not found in more than 75% of cases of chronic urticaria.
Another type of hives is cholinergic urticaria, triggered by emotions, heat, exercise, or change in temperature. Cholinergic type is different from the allergic type and is more fleeting in its appearance and disappearance. They are small (1 to 3 millimeters), pinpoint-like, raised wheals, surrounded by a large, intensely red rim. They disappear without treatment in 30 to 60 minutes, but tend to recur in susceptible individuals. Why some people react with hives to stress is not known. Despite the most diligent of efforts, the cause is not found in more than 75% of cases of chronic urticaria.
Hives Can Be A Sensitive Skin Symptom
Hives are itchy raised welts or plaques that may play a sensitive skin role as part of increased immune reactivity and immunoglobulin E (IgE) action in sensitive skin. This role can be substantial in certain sensitive skin people. Hives, also called urticaria, appear as red, itchy, swollen areas of the skin that can vary in size and can show-up anywhere on the body. About 20% of people will have hives at least once in their lifetime. Acute hives are often due to a viral infection, perfume, drug, food, latex, or other allergen. Some have chronic hives that occur daily for months to years. Constant scratching, direct pressure, or long-term anxiety may aggravate chronic hives. Atopic patients can experience acute hives due to their increased Ig E levels. However, the incidence of chronic hives is not increased in atopic patients. So, sensitive skin people can experience hives but hives do not necessarily mean that the patient has atopic dermatitis. Hives can occur separately from atopic dermatitis and separately from any other form of eczema. Though they are both symptoms of sensitive skin, you should think of hives and eczema as two different entities as hives have a different mechanism than eczema.
You can diagnose hives with a simple skin test. Take a blunt point such as a Chinese chopstick. Using the chopstick, draw an “X” on your bare back. Wait a minute. If you see a red elevated “X” on your back, you have “dermatographism” which is a sign of hives.
 Histamine Release In Sensitive Skin
Histamine Release In Sensitive Skin
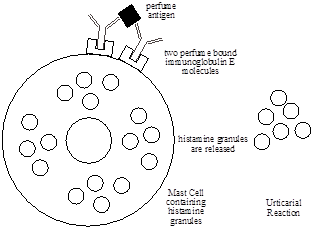
Hives are the result of a biochemical called “histamine” in the upper skin layers. Histamine is responsible for swelling, redness, and itching in hives and is usually stored in immune cells called “mast” cells. Histamine is vasoactive which means it causes blood vessel dilation (vasodilation), increased blood vessel permeability, and movement of proteins and fluids from inside the blood vessel, to outside of the blood vessel. As a result, the skin tissues swell with fluid, the skin turns pink, you feel itchy, and you see hives. Several known “triggers” may release histamine from mast cells. Most but not all are induced by IgE. To release histamine, two IgE molecules bind to a mast cell. An allergic particle then binds to both IgE’s. This combination turns on a set of enzymes and histamine is released. A mosquito bite causes histamine release by IgE and is a good example of acute hives.
Known Histamine Triggers
Medications known to cause hives include aspirin, ibuprofen, and similar anti-inflammatory drugs. High blood pressure medicines known as ACE-inhibitors, laxatives, and painkillers containing codeine are also known to cause hives. People can develop hives after eating certain foods including nuts, eggs, shellfish, soy, wheat, or milk. Cheese, wine, tomatoes, strawberries, and chocolate can also cause hives. Sulfite salts, metabisulfites, and dyes can cause hives. Perfumes of any kind can cause hives. Pollens, molds, and danders can cause hives. Certain women are allergic to their own progesterone. Viral, parasitic, or bacterial infections can cause hives. Hives can also result from an outside source such as rubbing of the skin, exposure to cold, heat, physical exertion, exercise, pressure, or direct sunlight.
How To Treat Hives
With increased immune reactivity, sensitive skin people may develop hives easier than non-sensitive skin people. The most important goal is to identify the actual cause of the hives. This may be impossible. But, whenever there’s an identifiable trigger in hives, that triggering agent should be eliminated. Until the offender is eliminated, a physician may prescribe antihistamines to relieve symptoms. It’s interesting to note that atopic dermatitis patients feel better if they take daily antihistamine therapy. This shows the importance of IgE in atopic dermatitis. One common over the counter antihistamine is Benadryl™. Benadryl™ may be fine, but can cause drowsiness. Dr. Jacobs can prescribe special prescription antihistamines that are less sedating. The subject and treatment of hives is very complicated. Most will not, but certain sensitive people will need to visit a dermatologist or an allergist for complete evaluation and management of hives. As part of this educational sheet, the subject of hives is introduced for your education. You should be aware that certain allergens and factors cause histamine release. Simple avoidance of these allergic items is usually the first and best way to control hives in sensitive skin people.
Photos

