Eczema
UNDERSTANDING
ECZEMA
You
or someone you love may have eczema. But what is eczema? And what can you do about it? How do you control the
itch? Stop the rash? How do you start back on the road to comfort
and recovery? This patient education sheet
was written to help answer questions and concerns like these. Dr. Jacobs wants
to help you understand eczema because, by understanding the disorder, you can
take your first step towards living comfortably within your skin. By the way,
the words “Eczema” and “Dermatitis” mean the same thing. They can be used
interchangeably, and, like “water” and “H2O,” they are synonymous.
What is
Eczema?
A
famous Austrian doctor named Hebra described it well
years ago when he said, "Eczema is
what looks like eczema." Sound confusing? It's not really. What Hebra meant was that
eczema is not defined by what causes, it, but by what it looks like. You see, eczema is really just a general term covering a group of 10 or
12 skin disorders that all look alike, but are caused by different factors. But
interestingly, even though different factors can cause each type of eczema,
there is one common factor that is shared by all types of eczema. That factor
is: Each type of eczema has, in some way, a damaged, dysfunctional, or
perturbed skin barrier. To learn more about the skin barrier, and, when it comes
to eczema, the skin barrier’s role in “keeping the peace,” Please take a few
minutes to read the patient education sheet titled, “Dry Skin and Skin Barrier
Education,” and my booklet, “The ABC’s of Dry and Sensitive Skin.”
Quite
simply, eczema, like a fire, begins when the skin barrier is damaged or
perturbed, allowing the passage of allergens, toxins, and infectious agents
that call forth white blood cells, dryness, and the whole eczematous
inflammatory process that results in what you see and what Hebra descrided as "Eczema is what looks like
eczema."
What Does
Eczema Look Like?
Eczema
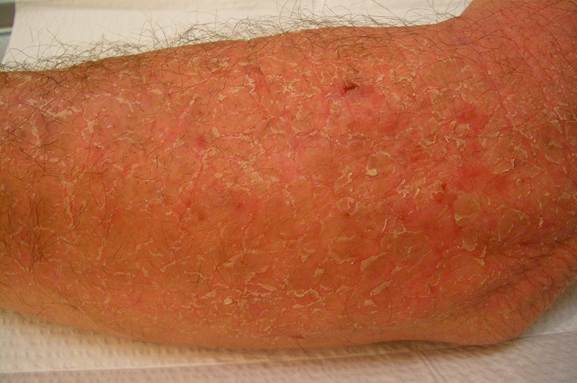
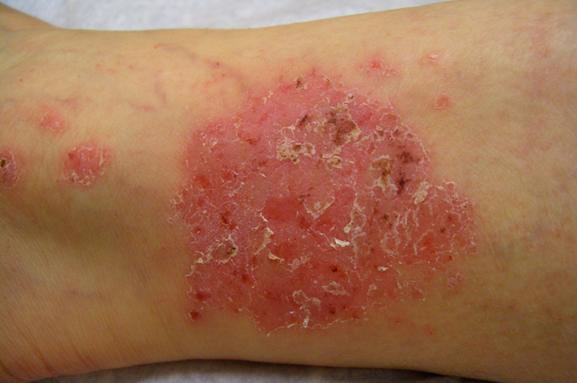
has three different stages, each with its own distinctive features. You may experience only the first stage, only
the first and second, or you may go through all three stages. Dermatologists call these three phases of
eczema acute, subacute, and chronic. Acute eczema is
stage number one, starting with some redness, swelling, and itching. The redness quickly changes into blisters
which, when they break, promptly begin oozing or weeping. The itching can become severe at this point,
but you must try hard not to scratch. Scratching only intensifies the itching and worsens your condition.
WHAT TYPES
OF ECZEMA ARE MOST COMMON, AND, WHAT ARE THEY CAUSED BY?
Contact
Eczema or Dermatitis
As
the name "contact" implies, this type of eczema is the result of an
outside irritant making contact with your skin. Contact eczema is usually an allergic reaction. A person only rarely develops a rash after
only one contact. This is the nature of
allergy. The first contact almost never
irritates. It is the second or the third
of fourth or tenth or hundredth contact that irritates. Sometimes the rash develops with the next
encounter, and sometimes it takes years for the skin to suddenly become
sensitive to a certain substance. It
also works the other way what a person reacts to now may, after a few years,
hardly bother him at all he has "outgrown" his allergy. Sometimes the
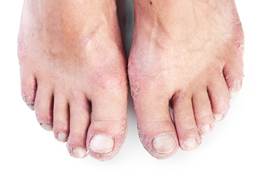
placement and the shape of the rash can give a clue as to the cause. For example, sensitivity to a certain dye in
shoe leather will affect only the tops and sides of the feet. Or, a rash due to a low shrub could mark the
legs in a horizontal streak. Substances that commonly cause reactions in some
people, or may be causing a reaction in you, are:
- plant (like poison ivy)
- foods (like nuts and shellfish)
- industrial chemicals
- medications applied to the skin
- perfumes
- cosmetics
- fabrics
- household cleaners
- polishing agents
Almost
anything can cause contact dermatitis. A person is never allergic to something
the first time they use it. It takes many repeated exposures before the body
can develop a true allergy to a substance. Often, a person will say, “Dr.
Jacobs, I can’t understand how I can be allergic to my perfume, I have been
using it for 10 years.” Dr. Jacobs explains that the person has used the
perfume for 10 years, and has finally acquired an allergy due to repeated
exposure. The same holds true for allergic reactions to all things. A person
needs to be exposed to a substance repeatedly before an allergy can occur.
Most
of the time, Dr. Jacobs can take a simple history and can find out what you are
allergic to. Sometimes, Dr. Jacobs may have to order blood tests or do special
skin testing to determine your allergies.
Primary
Irritant Eczema or Dermatitis
This
form of eczema is a close cousin of contact dermatitis. The difference lies in the fact that primary
irritant dermatitis is not an allergic reaction the first contact, if it is
long enough and strong enough, will cause eczema to develop in everyone. Examples of substances causing primary
irritant dermatitis are strong acids and alkali (like battery acid and Bleach),
solvents (like turpentine), and strong soaps and detergents.
Atopic
Eczema or Dermatitis
This
type of eczema differs from the fist two that we've just discussed because it
is a hypersensitivity that can be amplified by contact. It is a tendency or disorder that runs in
families and often occurs together with other types of allergic disorders. Infants, for example, who have eczema may
outgrow it by the age of 5 or 6 but often develop asthma or hay fever
later. Atopic eczema is a chronic type
of dermatitis, but acute flare-ups are often triggered by a number of factors,
a few of which are heat, cold, rapid changes in temperature, sudden sweating,
stress, and fatigue.
Eczematous
Dermatitis
An
umbrella title, “eczematous dermatitis” covers any form of eczema not easily
classified into the preceding categories. These eczemas or “dermatitides”
(plural of dermatitis) can be
due to many different factors and appear in many different patterns. For example, infective eczematous dermatitis
is a rash developing in the patch of a draining bacterial, fungal, or viral
infection. In contrast, stasis
dermatitis, a rash stemming from poor circulation due to varicose veins. Stasis
dermatitis usually occurs in swollen legs with poor circulation. Xerotic eczema or nummular eczema occurs in skin that is
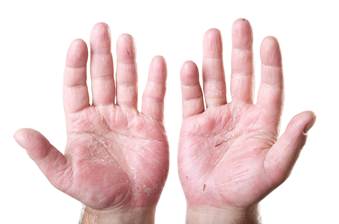
chronically dry and inadequately moisturized. Hand eczema may occur from
frequent hand washings or from use of strong solvents at home or work. Eczemas
may occur in a variety of different patterns, and may require different
treatments.
AT
WHAT AGES IS ECZEMA COMMON, AND, WHAT BODY PARTS ARE USUALLY AFFECTED?
Eczema
can occur at any age and on almost any part of the body, with some areas being
more sensitive than others. Contact eczema usually affects the area where
contact was made with an irritating substance. Some good examples are diaper rash in infants, detergent hands in
adults, or a poison ivy reaction in any age group.
WHAT
IS THE TREATMENT FOR ECZEMA?
How
to Care for Sensitive Skin,
Atopic
Skin, Allergic Skin, or Eczematous Skin
Dry
and sensitive skin problems are among the most common reasons for coming to the
dermatologist. Dry skin is a problem for many people, especially in cool
weather when the air is dry and furnaces are turned on. How does dry skin
develop? Normally, your skin moisture is protected by your skin barrier lipids
filling the intercellular spaces between skin cells. Soap can wash these
protective bio-oils away, and your skin can lose moisture. Dry air further
causes the skin to lose moisture, and your dried skin can scale, flake, and
crack. The tiny cracks in the skin are also called “fissures” and occur within
the lines of the skin. As tiny dry fissures deepen within the skin lines,
inflammation and sometimes infection develops, leading to a medical condition
called: asteatotic or xerotic eczema, the medical names to describe severely dry skin. The words “eczema” or “dermatitis”
are the same and refer to inflamed skin. Eczema or dermatitis can be due to
allergic or irritating substances, infections, low oxygen, drugs, and dryness.
The chapped, cracked “eczematous” areas may become irritated and itchy. The
skin can appear scaled like fish scales, a condition called “icthyosis.” If sensitive skin is a problem, the dry
eczematous skin rash can form patches that resemble ringworm. This condition is
called “nummular” eczema. At times, the skin may peel like parchment paper.
Other times, the skin may appear red and flaky. If low oxygen is a problem as
with swollen or varicose legs, the condition is called “stasis dermatitis.” If
asthma, allergies, or hay fever is in the family history, the dry skin problem
may be magnified. This dry skin condition is called atopic dermatitis. The dry
skin care principles explained in this handout apply to all people who suffer
with dry skin, sensitive skin, allergic or atopic skin, icthyotic skin, nummular skin, or any type of eczema, including stasis.
Moisturization
The
most important part of therapy is to first restore moisture to the skin. It’s
like filling a dry lake bed. Skin lubrication will restore your skin’s
moisture. How is this done? Just add water! Water alone will briefly moisturize
your skin, but the new moisture is soon lost to the air by routine evaporation.
How to prevent evaporation? Creams and ointments provide a protective film or
coating of oil that prevents skin water from evaporating. The oils can also
seep deep into the intercellular spaces and can temporarily refill your skin
barrier so that it can once again function. This protective oil coating
prevents dryness. Any type of oil can prevent water loss. Bath oils can be an
effective way to prevent loss of moisture. You can rub bath oil onto your skin
after a shower or bath. You can add it directly to your bath water: CAUTION:
Slippery tub! When applying bath oil directly to your skin, first, soak in your
tub and wipe your skin with a moist towel. Second, pour a small amount of bath
oil into your hands. Liberally spread it around. Three large tablespoons of
bath oil is enough for the entire body of an average adult male. If you prefer
to use bath oil in the tub, after you have soaked for 10 minutes, add a
tablespoonful of oil to the bath water and soak for 10 to 20 minutes more. Do
not use soap, as you will be cleansed by soaking in the oil-water combination.
After soaking, pat yourself dry with a damp towel. Enough bath oil will remain
on your skin to prevent moisture loss. You can ask your pharmacist to show you
OTC bath oils or mineral oil. If you don’t like bath oil, you can moisturize
with OTC Cetaphil Moisturizing Cream or plain
Vaseline with good results. Sesame oil is also nice. The most important point
to remember: Any skin lubricant is best applied after your skin has been wettened in the bath or shower, so as to trap and hold
moisture in. Think of yourself as a bone dry sponge that has been soaked or
dipped in water. The sponge is then dipped in oil to tightly seal the moisture
in. Here is a recipe for an excellent home made moisturizer: Mix one pound of
Vaseline ointment with sixteen ounces of any fragrance free mineral oil. Add a
small amount of pure water to your liking. Mix them together, well, with an
electric mixer. Apply liberally to your body each day after your bath. You will
find this recipe to be effective and economical.
Treating the
Dry Skin Rash
When
dry skin has developed into an itchy rash, a cortisone cream or ointment
usually brings quick relief. The cortisone may be applied liberally to the rash
and deeply massaged in, usually at bedtime, or after bathing, and one or two
other times during the day. As your rash improves, the cortisone is decreased.
Remember, dry skin requires topical therapy. Many patients would like to treat
their dry skin with either a pill, an injection, or
diet. Some patients have asked if fat intake improves dry skin. Excessive fat
consumption can cause poor health. Please remember, when treating dry skin,
there is no safe substitute for conscientious topical moisturization.
If you want an oral cure, water is the best oral substance to help with dry
skin. Pills aren’t available. Topical care is best. First, soak the water
inside. Second, prevent evaporation with a film of oil.
Soap
Soap
is bad for dry or sensitive skin. Dial, Zest, Lever, Safegaurd,
Ivory, gels, and Irish Spring are among the worst. Soap removes skin oils
needed to hold in moisture. If oils are removed, the skin develops cracks,
fissures, and dry inflammation. Soap should not be used on dry or sensitive
skin. Most of us use far too much soap. Actually, plain water is often just
enough to cleanse the skin. If you can't live without soap, it's OK to use Dove
soap for your face, feet, armpits, and groin.
Avoid
Allergic Items
Sensitive
skin can become itchy when exposed to allergic type substances such as
perfumes, dyes, conditioners, powders, anti-perspirants,
hair sprays, grasses, plants, fragranced products, shampoos, unrinsed laundry detergents, fabric softener sheets, dog or
cat hairs, carpets, chemicals, Aloe Vera, PABA, detergents, acrylic nails,
polishes, nickel, elastic, latex, etc. Hair conditioners can induce itch!
Please avoid perfumes.
Bathing
Persons
with dry skin may bathe
~ or shower once daily:
1.
Use no soap on dry or sensitive skin areas. You may use mild Cetaphil or Aquanil soapless soaps, instead of soap.
2.
After bathing, thoroughly lubricate your skin using one of the methods
described in this educational sheet.
3.
After your bath, you should not towel dry. Wipe off the water with your hands,
then, apply a thin film of moisturizing cream to your entire body. This film
will seal in your new moisture.
4.
For shampoo, use OTC fragrance free DHS Clear Shampoo.
Long-term
Control
Dry
or sensitive skin is usually a long-term problem that may recur often,
especially in winter. When you notice your skin getting dry or itchy, resume
your lubricating routine, proper bathing technique, and avoid soap. If you are
a dry or sensitive skin person, avoid allergic items, especially perfumes and
antibacterial soaps. Aim to restore your protective skin barrier lipids.
What is Dry and Sensitive Skin?
What is dry and sensitive skin? Dry skin is common
problem, especially in cool weather when hot furnaces are turned on and the air
is dry. Young and old, infants and adults, millions of people suffer with dry
and sensitive skin. It may be you or your spouse, your children, your parents,
or even a friend. At highest risk are babies, seniors, diabetics, frequent hand
washers, eczema prone people, atopics, psoriatics, and people on water pills, acne meds, or
wrinkle creams. These people usually suffer with dry and extra sensitive skin.
If you look in the dictionary, there is no good definition
for the term" sensitive skin," but those of you who have it sure know
what it is. Sensitive skin dries out ever so easily, can ignite like a hot
match, and any allergic thing can set it off. If this skin type is neglected
and exposed to soap, dry air, and allergens, simple dry skin can deteriorate
into itchy eczema or the "Dry Skin Rash." Eczema, the Dry Skin Rash,
and most dry and sensitive skin problems can be traced to an easily damaged
skin barrier located in the upper layers of the skin. Microscopically, the skin
barrier resembles tiny bricks and mortar. Here is a simplified diagram of the
human skin barrier.
If you are a dry and sensitive person and you neglect your
skin barrier, you will have problems forever. The truth is, your skin barrier
needs daily care, but ironically, most dry and sensitive people are unaware of
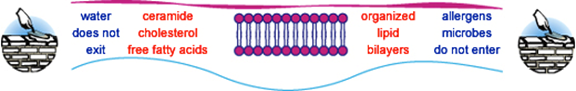
their skin barrier organ. A well-tuned skin barrier will keep body water inside
and will prevent allergens and microbes from entering your body. The
"bricks" are the corneocyte skin cells. The
"mortar," situated between skin cells, is made of three lipid-oils:
Free fatty acids, ceramide, and cholesterol. For
normal skin barrier functioning to occur, the three lipids must be
"organized" into precise layers called "lipid bilayers."
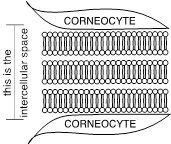
Here is an example of well organized, healthy, skin
barrier lipids:
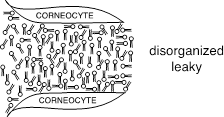
Here is an example of disorganized, unhealthy, skin
barrier lipids:
How Do You Get Dry Skin?
If cholesterol, ceramide, and
free fatty acids are stripped away as with excessive soap use, the lipid
bilayers will break down and the skin barrier is damaged.
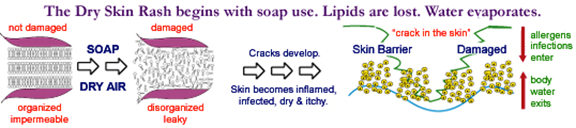
In this depleted state, the skin barrier will leak, and
thus, water will evaporate, allergens will penetrate, and microbes can enter to
infect. The skin becomes dry, inflamed, and infected. A rash ensues: The Dry
Skin Rash. Help! Some people try calamine, but dry calamine does nothing for
dry skin. Some people head to the shower and scrub their bodies with soap. This
only adds fuel to the fire. Hoping for relief, some splash rubbing alcohol all
over their lipid-depleted body.
They don't realize that soap and alcohol are only
stripping more lipids and causing more skin barrier damage. Finally, the dry
person goes to a local urgent care and gets cortisone pills. But, cortisone is
only a short-term fix for a long-term skin problem. What this suffering dry and
sensitive soul really needs is the ABC Skin Care.
|
||||||||||